The Disease
Norwalk virus causes viral gastroenteritis, which is also
known as acute nonbacterial gastroenteritis, food poisoning,
food infection, stomach flu, and winter vomiting disease.
A Norwalk virus infection results in illness 24 to 48 hours
after exposure, and symptoms last from 12-48 hours. Symptoms
are generally mild and self-limiting. Serious illness is rare,
and is usually associated with dehydration and/or electrolyte
imbalance in elderly, disabled, or immunocompromised individuals.
Illness is characterized by the abrupt onset of vomiting and/or
non-bloody diarrhea; abdominal cramps are common. 25-50% of
patients report headache, nausea, malaise, muscle aches and
low-grade fever. It is important to note that there are other
organisms such as rotaviruses which also cause viral gastroenteritis.
Unlike rotaviruses, Norwalk virus infection is more frequent
in older children and adults than in infants and toddlers.
 |
 |
Noroviruses enters the body by the oral route and travels
to the small intestine through the stomach. Virus replication
occurs in the mucosal epithelium of the small intestine. This
results in the broadening and flattening of the villi, damaging
mucosal epithelial cells. Noroviruses do not appear to infect
the cells of the large intestine. The exact binding site that
Noroviruses attach to the epithelial cells is still being
investigated. It is most likely that Noroviruses bind to a
very specific cellular surface protein, which is not being
expressed in animal models or cell lines.
New research suggests that there is a connection between
Norovirus infection and a person’s blood type. A, B,
and O phenotypes are determined by the presence or absence
of carbohydrate antigens on glycolipids and glycoproteins
found on the surface of mucosal epithelia as well as RBC’s.
In this study, individuals with type O phenotype were found
to be most susceptible to Norovirus infection. Individuals
who express type B antigen (B and AB phenotypes) were at decreased
risk of infection. When these B and AB phenotypes were infected,
they were more likely to be asymptomatic.
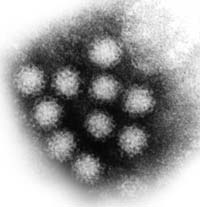 |
Identification of Noroviruses can be made
using electron microscopy since Noroviruses have a very
characteristic morphology. This technique is only effective
using stool specimens from infected patients within the
early stages (within 72 hours) of illness, when large
amounts of virus (106 – 107)
are shed. Virus samples should but kept at 4°C and
not be frozen, as this destroys the morphology of the
virus. |
Reverse transcription polymerase chain reaction (RT-PCR)
can be used to detect the presence of Norovirus nucleic acid
such as segments of ORF1 which codes for the RNA-dependent
RNA polymerase. This detection method is very sensitive (102
– 104 viral particles/mL) and can be used
to detect multiple strains of Noroviruses. Due to the specificity
of this test and the variability between virus strains, there
is always a chance that the RT-PCR primers will not recognize
certain strains of Noroviruses.
Serological assays can also be used to detect the presence
of Norovirus antigens. Genetically engineered strains of baculoviruses
express Norovirus capsid proteins that self-assemble into
virus-like particles. These particles can be used to generate
Norovirus-specific antibodies from animals for use in immunoassays.
Serum specimens from patients must be drawn at the proper
times, and testing is restricted to the limited antigenic
types (expressed in baculoviruses) available. For IgG assays,
acute-phase specimens are taken with the first 5 days of symptoms
and convalescent-phase specimens are taken from the third
to sixth week after resolution of symptoms.
Antibiotics are ineffective against Norwalk virus or any
other virus for that matter. Maintaining adequate fluid intake
to replace losses from vomiting or diarrhea is important.
The use of oral rehydration solutions (ORS) may be recommended
by physicians. These are available in pharmacies without a
prescription.

|