|

March 2002
Presented by: Dr. D. Yamamura1 and Mr. L. Wilcox2
1MDS Laboratories and 2Hamilton
Regional Laboratory Medicine Program

A previously healthy 9-year-old female was admitted to Children's
Hospital with a 10 day history of fever up to 103ºF and headache.
The patient developed a raised red rash with some pustules 7 days
prior to admission beginning on her lower extremities and soles
of her feet progressing to involve her upper extremities, palms,
face and trunk. Multiple joints involving her right hand, left hand,
right elbow, left wrist, left shoulder and bilateral knees and ankle
joints were red and swollen. The polyarthritis was asymmetric and
migratory. The patient denied any history of arthritis. There was
no preceding dairrheal or respiratory illness. The patient was not
sexually active and had not travelled. There was no significant
past medical history. A maternal aunt had rheumatoid arthiritis.
The patient was on Acetaminophen and Ibuprofen. All members of her
family had a recent upper respiratory infection. The patient had
a pet rat.
On physical examination, the patient appeared toxic and listless.
She had temperature of 36.9ºC and had an elevated heart rate.
The respiratory and cardiovascular examination was unremarkable.
Swelling, erythema and decreased ROM were seen in multiple joints.
Pustular lesions were seen on the soles of her feet. There was no
enlargement of her lymph nodes, or lesions in the oral cavity.
Laboratory investigation revealed that the patient had a WBC 8.3,
Platelets 328, ESR 85, CRP 168, and a negative ASOT. Rheumatoid
factor was normal. Joint aspirate of her knee showed 45.5 x 109
nucleated cells/L with 89% neutrophils. One of 2 sets of blood
cultures using the BACTEC 9240 (Bectom Dickson Microbiology Systems)
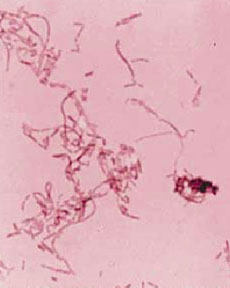
became positive after 28 hours of incubation. The gram stain revealed
a moderate to large, pleomorphic gram negative bacilli (GNB) with
long filaments and irregular swellings (Figure 1). Aspirate of the
right knee did not reveal any organisms by gram stain and the culture
was negative. A pleomorphic GNB was seen on the gram stain of a
swab of a pustule on the right foot.
The patient was treated with intravenous penicillin and gentamicin
and improved clinically. A transthoracic echocardiogram did not
reveal endocarditis. The patient was discharged home on amoxicillin.
Results from further microbiology investigations are summarized.
The blood culture was sub-cultured to sheep blood agar (SBA) incubated
anaerobically, chocolate agar (CA) incubated in 5% CO2, and
MacConkey agar (MAC) with crystal violet incubated aerobically.
No growth was seen on MAC or CA. Pinpoint growth was seen at 48
hours on SBA. The colonies were round, smooth, and gray. Initial
work-up revealed a catalase and oxidase-negative organism. No reaction
was seen on standard biochemical tests. The organism was incubated
in supplemented thioglycollate broth (Figure 2). Further biochemical
tests were performed. A reference laboratory confirmed the identification.

- What are the possible infectious and non-infectious causes
of rash, fever, and polyarthritis? After viewing the gram stain
what are the most likely cause(s)?
- What zoonotic (animal) sources have been linked to this syndrome?
- In a routine microbiology laboratory, what further tests and
supplementation would aid in the diagnosis of this organism?
What reaction do you see with the thioglycollate broth and what
organism is most likely given the reaction? What other diagnostic
modalities are available to confirm the identification?
- What are L-forms and what implication does this have for treatment?
- What clinical complications have been reported with this syndrome?

 |
 |
|
Figure 1: Gram stained smear of isolate on blood
agar medium |
Figure 2: Supplemented Thioglycollate Broth |
|
|





